Publications
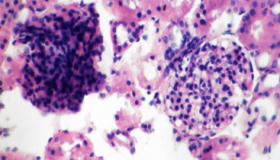
This monograph deals with one of the most actual problems of contemporary veterinary medicine – diagnosis and treatment of glomerulopathy and glomerulonephritis, the most common kidney disease in cats....
27.03.2015 / General 


|
WWW.VETNEFRO.RU Russian Scientific and Practical Association of Veterinary Nephrologists and Urologists
© All rights reserved 2025. Use of any materials from this site - is prohibited!
|